Effective Dose Calculation in PET/CT Imaging: Scientific Approaches and Clinical Safety
The content shared here is a summary of the article, for the full article: visit health physics
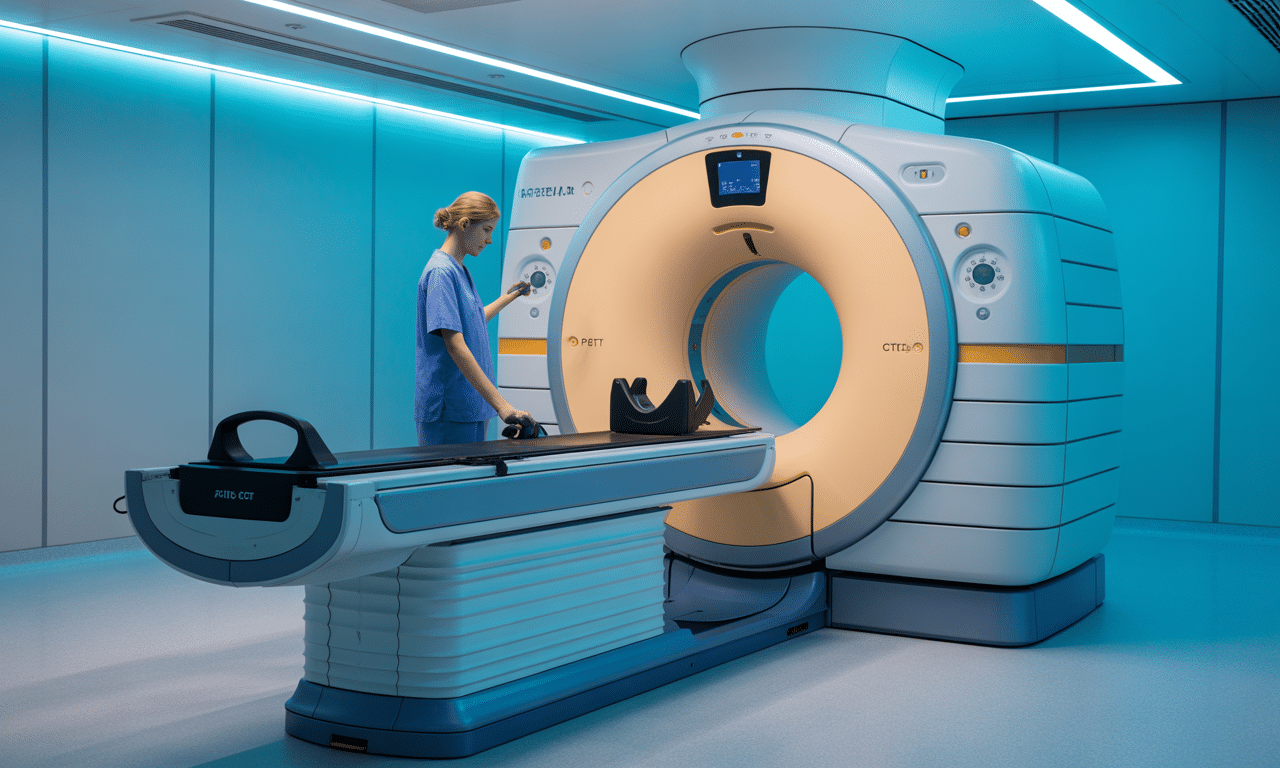
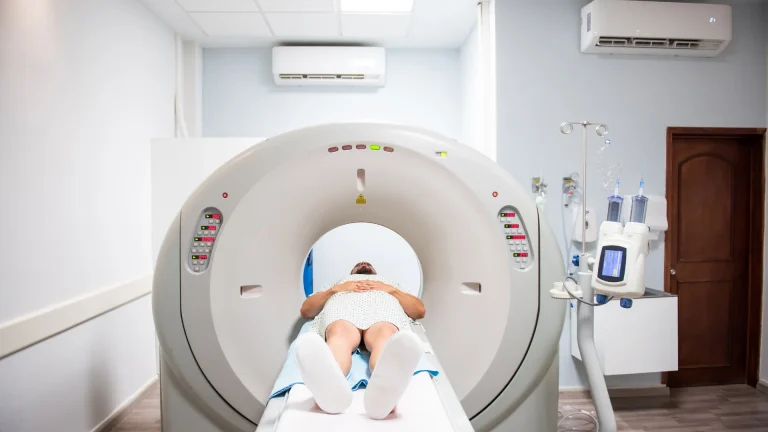
With the advancement of medical imaging technologies, the radiation dose received by patients has become one of the most important research topics in terms of both diagnostic accuracy and safety. PET/CT scanning methods, especially those used in cancer diagnosis, provide high-resolution images but also bring the risk of radiation exposure. Therefore, “effective dose estimation” is not just a technical measurement, but one of the key components of clinical safety.
This article describes the determination of the effective dose in PET/CT procedures using 18F-FDG and 68Ga-PSMA radiopharmaceuticals, the comparison of different software (OLINDA, IDAC-Dose 1.0, IDAC-Dose 2.1) and modern radiation safety principles.
The Importance of the Concept of Effective Dose
Effective dose is a concept that calculates the biological effects of ionizing radiation on the human body. It takes into account not only the amount of radiation received, but also how this energy is distributed to which organs. Each organ has a different sensitivity to radiation; for example, tissues such as the bone marrow, lungs, and thyroid are more sensitive, while skin or muscle tissues are more resistant.
The International Commission on Radiation Protection (ICRP) defines “tissue weighting factors” to balance this difference. The effective dose is obtained by converting the equivalent dose received by each organ into a general risk measure with the help of these factors.
The importance of effective dose in clinical applications stands out in two main points:
- Patient Safety: To determine if the total amount of radiation received by the patient is within acceptable limits.
- Protocol Optimization: To provide the highest diagnostic accuracy with the lowest radiation by comparing the dose efficiency of different imaging protocols.
Study Method and Software Used

This research, conducted at Yeditepe University Nuclear Medicine Department, included PET/CT scan data from 305 adult oncology patients . The two main radiopharmaceuticals used in the research are 18F-FDG (fluoro-deoxy-glucose) and 68Ga-PSMA (prostate-specific membrane antigen). Both substances are administered intravenously to the patient and follow different biokinetic models according to their involvement in organs.
Software Tools and Calculation Methods
In this study, the effective dose was calculated in comparison with different software tools.
| Software Name | Key Features |
| OLINDA/EXM | It is an advanced MIRD-based program that performs organ-level modeling and supports more than 1000 radionuclides. |
| IDAC-Dose 1.0 | It is a classic model developed based on ICRP 60 data. |
| IDAC-Dose 2.1 | Includes voxel models based on real human body geometry using ICRP 110 and 103 data. |
Each software uses different anatomical reference values, decay data, and mathematical algorithms. These differences cause changes in the calculated effective dose values. In the calculations, the PET and CT sections were evaluated separately and the total effective dose was defined as follows:
Total Effective Dose (EDtotal)=EDPET+EDCT
- EDPET: Represents the internal radiation dose from the radiopharmaceutical injected into the patient.
- EDCT: Represents the external radiation dose generated during the scan.
Findings and Interpretations
As a result of the research, the average total effective dose for 18F-FDG was calculated as approximately 25 mSv and for 68Ga-PSMA as 22 mSv.
Key Findings:
- The highest doses were obtained with OLINDA software, and the lowest values were seen in the IDAC-Dose 2.1 (ICRP 103) model .
- This difference is due to the new model’s use of more realistic texture representations and up-to-date decay data.
- The contribution of CT scan to the total dose was found to be 75% for 18F-FDG and 92% for 68Ga-PSMA . In other words, most of the total radiation received by patients is from CT.
The Evolution of Tissue Weight Factors

Tissue weighting factors used in radiation dose calculations refer to the contribution of each organ to the risk of developing cancer. With the transition from ICRP 60 to ICRP 103, these factors have been updated, for example, weight ratios for breast tissue and thyroid have been increased. Therefore, calculations with the new model often produce lower effective dose results because the relative contribution of some organs has changed.
Technical Perspective: Biokinetic Modeling vs. Software
Biokinetic modeling is used to determine how radionuclides are distributed in the body over time and in which organs they are retained.
- The energy release for 18F-FDG is particularly intense at the heart wall and bladder wall .
- In 68Ga-PSMA, the kidneys receive the highest dose because PSMA receptors are concentrated there.
Comparison of Software Models
| Phantom Type | Software | Explanation |
| Voxel Phantoms | IDAC-Dose 2.1 | Using three-dimensional voxel phantoms developed by ICRP 110, it creates representations of organs close to real human anatomy. This allows it to account for some energy transfer pathways that are ignored in MIRD-based simplified models. |
| Mathematical Phantoms | OLINDA/EXM | It uses mathematical (stylized) phantoms; This causes in some cases to more roughly estimate the energy transitions between organs. |
These differences become particularly pronounced in pediatric and gender-based calculations. For example, updating the reference data of the uterus and breast tissue in female patients leads to a lower total dose calculation of IDAC-Dose 2.1. Thus, patients can be followed up without overdose estimation.
Radiation Safety in Clinical Applications
Radiation safety is vital not only for patients but also for healthcare personnel. Therefore, accurate effective dose calculations ensure not only patient safety but also occupational safety.
Modern hospitals now automatically record the total dose received by each patient using “dose monitoring systems“.
Clinical Safety Approaches:
- Dose Monitoring Systems: Automatic recording of the total dose received by each patient.
- Software Integration: System integration of data from tools such as IDAC-Dose.
- Low-Dose Protocols: It allows radiation to be reduced by 20-30%.
- Legal Compliance: Meeting both legal and ethical requirements.
Conclusion and Future Outlook
This study shows that different software tools used in PET/CT applications can create significant differences in effective dose calculations. IDAC-Dose 2.1’s use of up-to-date ICRP 103 data provides more realistic and low-risk predictions of radiation safety.
Considering the effect of the CT component on the total dose, protocol optimization and AI-supported dose planning systems will be at the center of radiation management in the future.
“Effective dose calculation” is not only a mathematical value, but also the ethical responsibility of modern medicine. Each correct calculation contributes to a safer treatment process for a patient. As science advances, the power of unseen light will be harnessed in a more controlled and humane manner.